Editor's note: This post was originally published in February 2020 and has been updated for accuracy and comprehensiveness.
This is the 6th blog in our series on understanding cushion properties with the help of ANSI/RESNA and ISO standards. See part 1 here, part 2, part 3, part 4, and blog 5.
We’re continuing our series on understanding cushion properties with the help of ANSI/RESNA and ISO standards. So far, we’ve covered the pressure mapping test method and the method for measuring the depth of immersion. Today we’re looking at the horizontal force test, which is part of ISO 16840-2, and a shear force test method.
The NPIAP/EPUAP/PPPIA clinical practice guideline is clear about how shear forces at the interface between the body and a support surface can exacerbate internal tissue deformations that can lead to pressure injuries. It’s not just about the overall, external pressure from the normal/downward forces - the forces involved when someone is seated are actually very complex and multidirectional, with compression, shear, and tension all distorting the tissues. The support surface should minimize those deformations as much as possible. While it is important to reduce the overall external pressure on the body, minimizing the shear forces at the interface is also a critical intervention in clinical practice. By doing so, internal tissue stresses and strains can be further reduced. Thankfully, interface shear force is a value we can measure in the laboratory.
When shear forces are reduced by the cushion and cover design, it is also important to understand if any other seating goals are compromised. For example, it’s easy to visualize a very slippery surface that might be good for the tissues but might be too slippery for the individual to maintain their posture in the chair. This is where the horizontal force test comes in.
Below is a photo of the fixture for the horizontal force test. Similar to other ISO protocols, it begins by placing the rigid indenter, shaped like the buttocks, onto the cushion, with a specified downward force applied by adding weights. In this test, a cable pulls the indenter forward, and the force it takes to drag the indenter across the surface is measured. More force to pull the indenter may indicate the person will be fairly secure in their posture, where less force may raise a concern that they may be more likely to slide forward.

To enhance this test, the University of Pittsburgh added a shear sensor beneath the location of the simulated ischial tuberosity (IT) in order to get a localized shear force measurement in an area we know is vulnerable to pressure injuries. This gives an indication of what the tissues may experience. High shear forces indicate the tissues are tugged and distorted more so, and low shear forces indicate less tugging, with potentially a reduction in pressure injury risk from tissue deformation.

These objective test methods can be used to analyze the effect of a single variable, such as a cover design change. In the test results below, a cushion was tested for shear and horizontal force, with a standard cover and with a cover that was intended to reduce interface shear forces. You can see that with the standard cover, Cover A, the shear values increased as the body was dragged from 0mm-20mm. The test was then repeated Cover B, the “low shear” cover. The results show the shear force was dramatically reduced with Cover B. It appears the cover was accomplishing what it claimed. However, would the seated posture potentially be compromised?
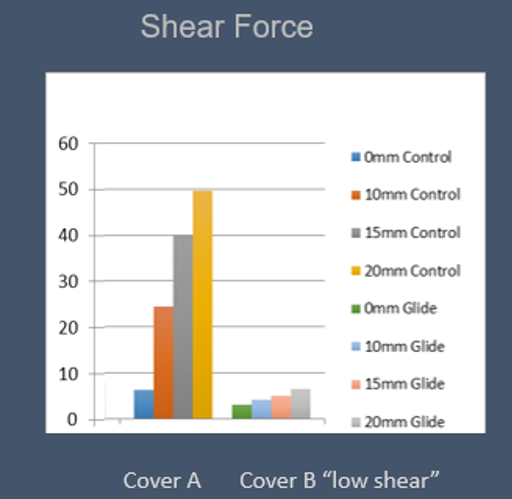
To answer that question, the horizontal force test was applied to the cushion with Cover A, and the force to drag the body 20 mm forward in the cushion was measured. The cover was then replaced with “low shear” Cover B, and the indenter was dragged again. The results from the horizontal force test were very similar.
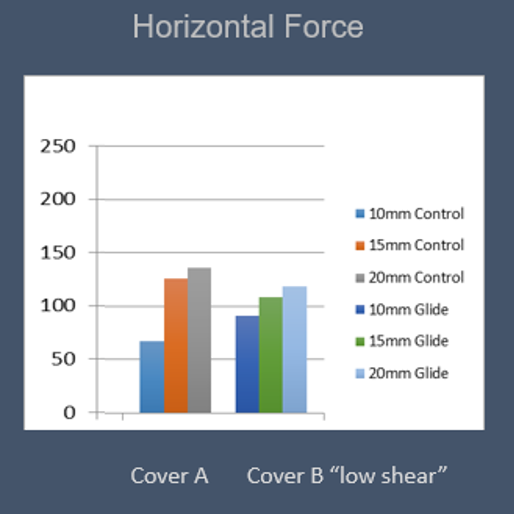
The takeaway from both tests is that the low shear cover, Cover B, did appear to lower the shear forces at the interface without compromising the ability to stay put in the cushion, potentially avoiding the effect of sliding forward. It’s extremely beneficial to have quantifiable, objective data from a laboratory analyze properties such as these and consider them in the overall clinical evaluation for the client.
Learn more about shear reduction technology that is offered in certain Permobil cushion covers.
For more information on the CPG, ANSI/RESNA Wheelchair and Related Seating Standards Committee, and the ISO standards for Wheelchairs and Wheelchair Seating, please visit:
https://guidelinesales.com/page/Guidelines
https://www.resna.org/AT-Standards/Wheelchair-and-Related-Seating-WRS
https://www.iso.org/committee/53792/x/catalogue/p/0/u/1/w/0/d/0
Images provided by the University of Pittsburgh Tissue Integrity Management Laboratory
 Kara Kopplin, B.Sc.Eng,
Kara Kopplin, B.Sc.Eng,
Chair of the ANSI/RESNA Wheelchair and Related Seating Committee, Director of Regulatory Science for Permobil
Kara Kopplin holds a B.Sc. in Ceramic Engineering from the University of Missouri-Rolla, U.S.A., bringing a unique and complementary materials engineering perspective to seating solutions. In her role as Director of Regulatory Science for Permobil, Inc., Ms. Kopplin actively contributes to the efforts of the International Organization for Standardization (ISO) and European Committee for Standardization (CEN) to develop object test methods for wheelchair systems and components. She is honored to chair the ANSI/RESNA Standards Committee on Wheelchair and Related Seating (WRS) in the US and encourages everyone to contribute to the development of these critical evaluation tools.

