Part 4 in our series about developmental milestones in early childhood focusing on mobility. See part 1, part 2, part 3, part 5, part 6, part 7, part 8, part 9, part 10, part 11, and part 12. Learn more about the Explorer Mini here.
As you see in this photo the young infant is weight bearing through hands, knees and toes. This proximal stability is what allows him to hold his head against gravity. This is a critical part of development. At two months of age this action is what facilitates head control and is linked to oculomotor control which is the foundation of visual skills. At this point the infant begins to develop visual fixations and is able to bring both eyes (controlled by six oculomotor muscles) together to stabilize his gaze. Infants who have not developed this trunk control lack the ability to gain full head and eye control. Without proximal control of the trunk and the development of eye gaze a child’s development will be greatly altered.
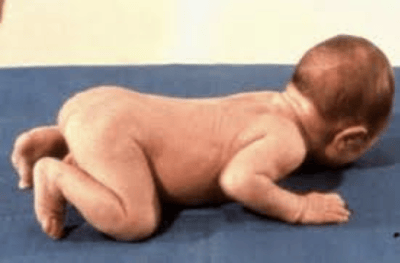
The seat surface and opportunity for weight bearing in the Explorer Mini aims to mimics this posture to augment the non-mobile infant.
So while a young child may not yet have full head control, the use of the Explorer Mini provides a supportive seat and weight bearing surface to encourage further development of the trunk, visual and vestibular system while providing proprioceptive input which stimulates co-contraction at the weight bearing joints, to help promote improved head control.
How sitting typically develops:
- 3-5 Months: Pre-sitting period, single postural muscles are activated. For an infant at this age they need postural support and opportunities for supportive sitting.
- 5-6 Months: A young child can sit with arm support.
- 7-10 Months: The leg, trunk and neck muscles are activated and cooperate in sitting and reaching activities.
- 9 Months to 3 Years: The young child has good modulation of pelvic muscles for a stable base of support.
- 3 Years and Beyond: The child needs less co-contraction and the use of neck muscles for postural control (6).
How does the Explorer Mini provide postures to mimic the stages a young child goes through for sitting?
For the non-ambulatory child, a stable base of support is realized in the Explorer Mini by many contact points and a wide base of support, such as is provided in a variety of positions by the adjustable seat and tray surfaces. In contrast in a device that positions the child in non-active sitting position, a child will typically assume a slumped posture with weight bearing behind the ischial tuberosities and no mechanoreceptors are activated.
The saddle seat surface of the Explorer Mini places the weight bearing in front of the ITs to facilitate weight bearing through the upper extremities and positions the pelvis in a forward/anterior tilt, with the hip position signaling the erector spinal muscles (or back muscles) to activate.
This device not only allows a young child to independently move, but it also promotes postures that may help them reach developmental milestones over time. Rather than limiting non-mobile young children to lay in a stroller or bed, we can use the Explorer Mini to help trigger muscle activation in postures that are safe and stable.
1.Hagert, E., Persson, J., Werner, M., & Ljung, B-O. (2009). Evidence of wrist proprioceptive reflexes elicited after stimulation of the scapholunate interosseous ligament. American Society for Surgery of the Hand, 34A. 642-651.
2.Henderson, A., & Pehoski, C., (2006). Hand Functions in the Child: Foundations for Remediation, 2nd edition. Mosby, Elsevier. St. Louis, Missouri.
3.Michelson, JD, & Hutchins, C., (1995), Mechanoreceptors in human ankle ligaments. The Journal of Bone and Joint Surgery. British vol. 77-B
4.Rosenblum, S., & Josman, N. (2003). The relationship between postural control and fine manual dexterity. Physical and Occupational Therapy in Pediatrics, 23,(4). 47-60.
5.Stavness, C., (2006). The effect of positioning for children with Cerebral Palsy on upper-extremity function: A review of the evidence. PT and OT in Pediatrics, 26,39-52
6.Westcott, S., & Burtner, P. (2004). Postural control in children: Implications for pediatric practice. PT and OT in Pediatrics, 24, 5-55.
7.Scheiman, M. (2011). Understanding and managing vision deficits: A guide for occupational therapists. Thorofare, NJ: SLACK Incorporated.
 Dr Teresa Plummer, PhD, OTR/L, ATP, CEAS, CAPS
Dr Teresa Plummer, PhD, OTR/L, ATP, CEAS, CAPS
Associate Professor in the School of Occupational Therapy at Belmont University
Dr Teresa Plummer, PhD, OTR/L, ATP, CEAS, CAPS is an Associate Professor in the School of Occupational Therapy at Belmont University in Nashville, TN. She has over 40 yrs of OT experience and 20 in the area of Assistive Technology. She is a member of the International Society of Wheelchair Providers, and the Clinicians Task Force. She is a reviewer for American Journal of OT and guest reviewer for many other journals. She has presented internationally, nationally and regionally particularly in the area of pediatric power mobility. She has authored journal articles and textbook chapters in the area of OT and pediatric mobility and access.

