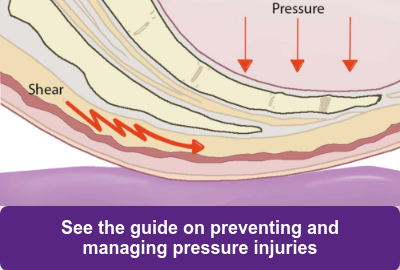
Part 1 in our Wound Care Guide series. Check out our comprehensive, digital Pressure Management Guide.
When we talk about wounds caused by pressure, we often only consider the pressure on our bottom. However, pressure can be created by any support surface that comes in contact with the body such as the:
- the cushion
- the back support
- the arm rests
- the head support
- the legrests
So, let’s clarify the definition of pressure when considering it from the seated posture.
Pressure is a continuous force applied on or against an object through direct contact. In seating, equipment such as the seat and/or back support surface is in constant contact with the body, creating peak pressures.
Peak pressure is a constant pressure directly under or against the bony prominences that will cause a pressure injury without proper pressure redistribution through appropriate cushion and back support choices. We will learn more about pressure redistribution methods in later blogs in this series. Peak pressures are commonly found at the ITs, sacrum, coccyx, and on the spinous process, injuring the skin and underlying tissue, muscle, and, in extreme cases, bone.
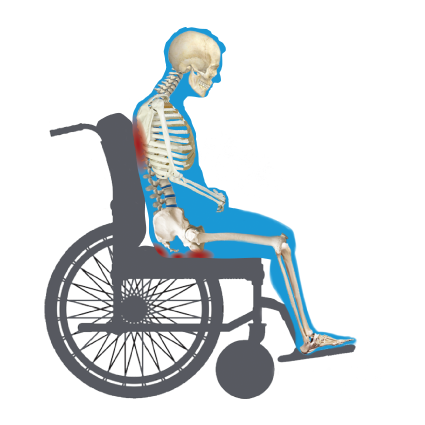
Where do peak pressures enter the body in a seated posture?
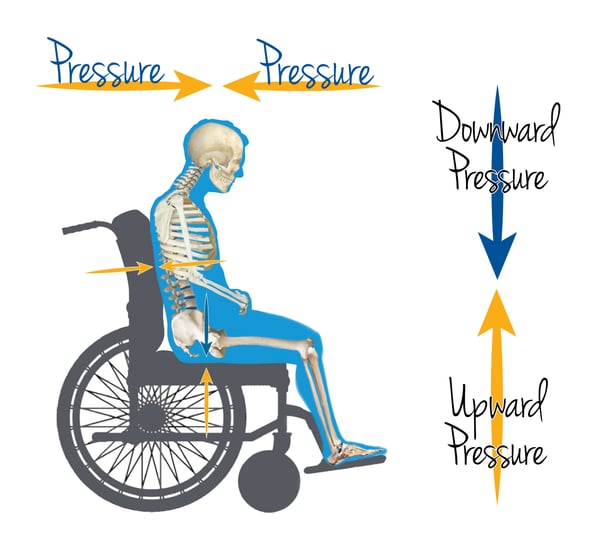
Pressure from a seated posture comes from:
- downward pressure from gravity
- upward pressure from the seat surface
- horizontal pressure along the spine from the back support
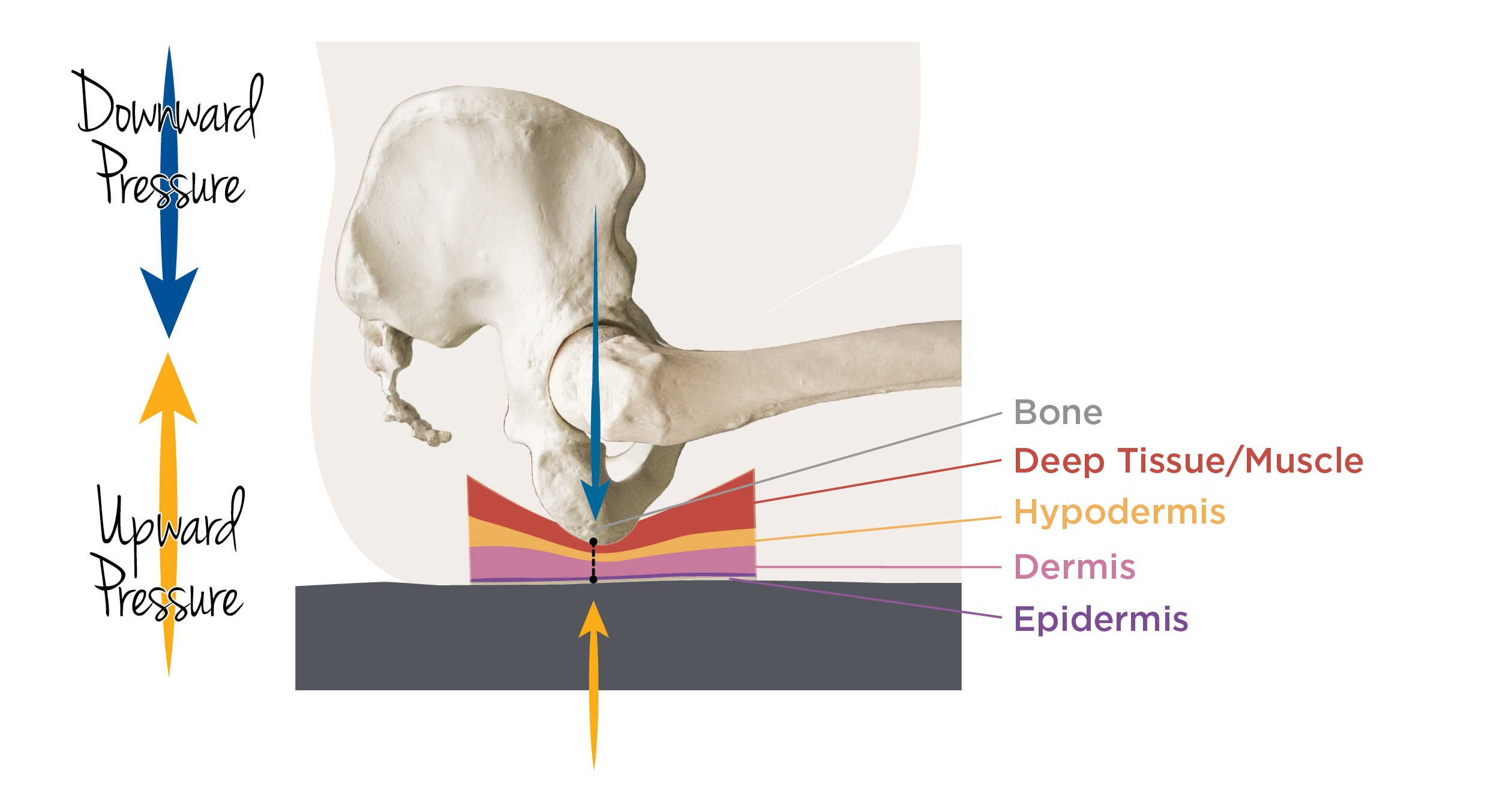
 When these peak pressures are not addressed through proper pressure redistribution techniques with the appropriate cushion and back support, the skin, tissue, and bone is compromised. Sustained loading against the back support and/or seat surface causes constant compression of that skin and tissue under a bony prominence, leading to a pressure injury. The degree of injury depends on the layers of skin impacted.
When these peak pressures are not addressed through proper pressure redistribution techniques with the appropriate cushion and back support, the skin, tissue, and bone is compromised. Sustained loading against the back support and/or seat surface causes constant compression of that skin and tissue under a bony prominence, leading to a pressure injury. The degree of injury depends on the layers of skin impacted.
Pressure Injury Stages
 |
Initially, it affects only the superficial epidermal layer, causing a reddening of the skin. Skin is still intact. |
 |
Eventually, the pressure moves into the dermis, breaking the skin open and causing an open wound. Blisters may appear. |
 |
Continued pressure damages deeper into the hypodermis, now affecting all three layers of skin. |
 |
Injury depth reaches the tissue under the skin, potentially penetrating to the muscle and bone. |
It is important that we as therapists, nurses, and doctors begin to understand the critical role that the seated posture plays in the prevention and treatment of pressure injuries. Permobil has developed a Wound Care Guide to help us clear up some misconceptions about pressure injury development and understand the role the seated posture has in total skin health.
Follow us as we highlight some of the hot topics through our 10-part blog series and explore issues such as:
- The BIG Misconception: a new cushion is all that is needed to prevent or heal a wound.
- Why should every patient be on a cushion?
- What are the methods of pressure redistribution?
- Why should we replace the sling back or straight back on a wheelchair?
- The importance of Seat-To-Back Angle (STBA) in pressure redistribution.
- Why should we worry about providing a more supportive, adjustable back support that will conform to the patient’s spine?
- Inside-out or outside-in wound development.
- The importance of trial equipment.

Ana Endsjo, MOTR/L, CLT
Clinical Education Manager LTC Division
Ana Endsjo has worked as an occupational therapist since 2001 in a variety of treatment settings. She has mainly worked with the geriatric population, dedicated to the betterment of the treatment of the elderly in LTC centers. Her focus has been on seating and positioning and contracture management of the nursing home resident. With this experience, her hope is to guide other therapists, rehab directors, nurses, and administrators through educational guides, blogs, webinars, and live courses in her role as Clinical Education Manager for the long term care division.