Part 1 in our blog series focusing on Pediatric Mobility Solutions and the TiLite Pilot.
It has been well established that the importance of self-initiated mobility is essential to a child’s development. The ability to determine when and where you would like to move impacts multiple body systems. This self-directed mobility can positively influence a child’s ability to locate and track objects in their environment, understand movement planning, improve communication, and enhance emotional and cognitive development. With the TILite Pilot, we are creating an opportunity to support these developmental milestones through self-initiated manual wheeled mobility.
In this four-part blog series, we are going to discuss some of the current limitations of pediatric manual wheelchairs, the way that a child propels a manual wheelchair, the importance of rear wheel access from the very first push, and address frequently asked questions. We will also explain how the design principles of the TiLite Pilot reduces the sacrifices one often has to make for small or young riders.
It is essential to start a child out with an appropriate manual wheelchair for independent mobility, because inherently a young child does not have the strength, endurance, or development to propel all day the way an adult would. But through optimal chair set-up, they figure out the movement patters and coordination needed. Starting them out right can set them up for long-term success in regards to shoulder biomechanics. If they are going to be using a manual wheelchair for long-term mobility, we can be aware of propulsion from the very beginning when the shoulder joint has not yet set-up patterns and positions that can be debilitating, so let's apply these same principles earlier to prevent shoulder impairments and preserve function. Oh, and don’t forget the chair should be fun and inviting to the child that may be experiencing wheeled mobility for the first time.
Limitations in Pediatric Mobility Options
When we think about traditional pediatric self-propelled manual mobility, we can all identify several limitations in the overall design. Typically, these are related to overall weight of the chair, configuration options, and incorporating growth that maintains wheel position throughout the time the child utilizes the manual wheelchair.
Often not only does the weight of the wheelchair equal the weight of the child, but the weight of the chair can even exceed the weight our youngest riders. In the adult population, a few pounds may not have as significant of an impact; however, when you’re talking about a weight ratio here of 1:1, pediatric mobility solutions should be as lightweight as possible.
If a family is able to obtain a lightweight chair, often it has to be custom made for each child. And while this type of wheelchair can be a great option for the pediatric population, there can be limits on the ability of the chair to grow along with the child. The chair being used is one of a kind, high-performance chair. This type of chair is usually not covered by traditional funding sources or if it is, it would not be replaced or grown through traditional funding sources. This can limit access and decrease longevity of the equipment for children and parents.
Managing chair stability through the wheelbase is another design challenge that gets compromised in pediatric self-propelled manual mobility. This is the distance from the front small wheel, or caster, to the back big wheel, or drive wheel. From the image below, we can see the chair is a little too wide for him, but what we really see from the side profile is the short wheelbase.
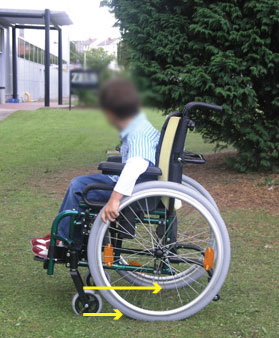
He’s going to have a lot of forward or anterior instability if he wants to reach to the ground or if he wants to transfer or crawl up the front of the chair because of the position of his body over the wheels. In addition, we do not have the ability to reposition him to improve wheel access. His weight/center of mass, at his stomach or pelvic area depending, is not well positioned over the rear axle. This manual wheelchair set-up with a short wheel-base (distance between big and small wheel) will result in a loss of forward stability as well as not setting up him up for successful push efficiency.
Another limitation we run into in the pediatric market is the additional weight that of seating components and accessories add to the overall weight of the chair. When we add a back support and cushion a lot of times those seating components, including the hardware, the plywood, the t-nuts, and all of the many components that go into our seating solutions can weigh just as much as the child. This results in a seating solution that actually adds a substantial amount of additional weight to the chair. These additions can negatively affect the ease and distance the child can push the chair, thereby not setting up the child for success.
In our last example, let’s take a look at the young lady in a traditionally available pediatric manual wheelchair who is ready to start increasing her independent mobility. For clarification, she is in a TiLite Twist which can be a good option for pediatric manual mobility. In this particular case, the wheelchair setup wasn't an ideal solution.
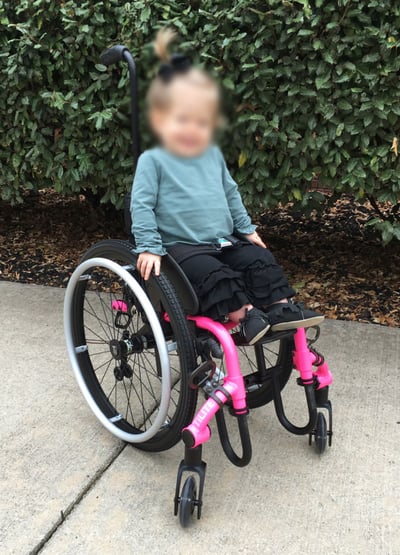
We don’t know the specifics of her case, but what we can assume is her treatment team provided this chair for her assuming that she will grow into the chair and be able to utilize the chair for years to come. However, it will only be once she grows into the chair that she will have more access to the wheel for pushing the chair, her feet will be supported, and she will have more forward stability. We don’t want to wait for our clients to grow to have an optimal manual wheelchair setup. We want to optimize positioning, posture, and push efficiency from the very beginning. When I look at her, I just want to take her great upright posture and move her down and move her back on that wheelchair frame, but unfortunately the design of the chair just really won’t allow us to do that.
From these examples, we can look at how limiting some traditional pediatric manual mobility solutions can be for our youngest riders. Next week we’ll be looking at the goals and physiology behind the design of the TiLite Pilot.
References:
Bornstein, M. H., Hahn, C.-S., & Suwalsky, J. T. D. (2013). Physically developed and exploratory young infants contribute to their own long-term academic achievement. Psychological Science, 24(10), 1906–17. http://doi.org/10.1177/0956797613479974
Lobo, M. a, Harbourne, R. T., Dusing, S. C., & McCoy, S. W. (2013). Grounding early intervention: physical therapy cannot just be about motor skills anymore. Physical Therapy, 93(1), 94–103. http://doi.org/10.2522/ptj.20120158
Marr, C., Seasman, A., & Bishop, N. (2017). Managing the patient with osteogenesis imperfecta: a multidisciplinary approach. Journal of multidisciplinary healthcare, 10, 145.
Sawatzky, B. J., Slobogean, G. P., Reilly, C. W., Chambers, C. T., & Hol, A. T. (2005). Prevalence of shoulder pain in adult-versus childhood-onset wheelchair users: a pilot study. Journal of rehabilitation research and development, 42(3), 1.
Slavens, B. A., Schnorenberg, A. J., Aurit, C. M., Graf, A., Krzak, J. J., Reiners, K., ... & Harris, G. F. (2015). Evaluation of pediatric manual wheelchair mobility using advanced biomechanical methods. BioMed research international, 2015.
 Jennith Bernstein, PT, DPT, ATP/SMS
Jennith Bernstein, PT, DPT, ATP/SMS
Regional Clinical Education Manager
Jennith Bernstein received her masters in Physical Therapy at North Georgia College & State University and returned to complete her transitional DPT at University of Texas Medical Branch in 2014. While at Shepherd Center, Jennith, initiated a “Seating Champion” program to improve the inpatient and day program clinicians understanding of complex seating, pressure management and skin protection as well as research reviews, advanced programming and adjustments. She was also part of a center wide multidisciplinary focus group for reduction of hospital acquired skin breakdown. Jennith has served as a volunteer teacher at the Universidad Mariano Galvez in Guatemala, instructing spinal cord injury curriculum as well as seating and mobility. Jennith has presented at national conferences such as RESNA, ISS, and the APTA NEXT conference. Jennith has been a practicing PT for 12 years and spent the last 10 years at a model SCI center (Shepherd Center) in Atlanta, Georgia. Jennith joined Permobil as the Clinical Education Manager for the Central Region in 2016.

