Part 3 in our series 24 Hour Positioning: Why Wheelchair Seating Can Only Do So Much by guest author Tamara Kittelson-Aldred, MS, OTR/L, ATP/SMS. See Part 1 and Part 2.
In Part 1 we discussed three primary postural orientations and our American seating practitioner tendency to overlook posture in lying. The work of Fulford and Brown demonstrated in Part 2 that gravity, asymmetrical postures and time combine to distort the shape of a person’s body.
With educated eyes we can clearly see the link between lying and sitting. We all have postural tendencies – for instance one side is stronger or more flexible than the other. In fact, functional activities often hinge on asymmetry. But asymmetrical postural tendencies tend to be even more pronounced in people with neuromuscular conditions.
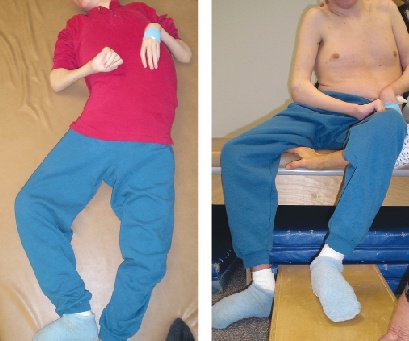
Figure 1: Supine Posture Figure 2: Sitting Posture
Imagine a person lying for hours in the same or a very similar posture. A person often shifts position slightly over a period of time but with a limited movement repertoire, so in the end there is never much variety. Soft tissues on one side shorten while lengthening on the other side. Meanwhile, gravity is an ever present force flattening the body against the support surface. Remember Noreen Hare’s “human sandwich” from Part 1? Joint ligaments can stretch as the extremities seek a support surface, sometimes enough to contribute to joint dislocation – especially if the joint is already at risk. The chest, which is a highly flexible structure comprised of both bone and cartilage, will also be affected (Hill & Goldsmith, 2010). In those who sleep supine or prone it may compress symmetrically so that the chest becomes wider and flatter, or conversely narrow and deep in people who are side sleepers. If rotation enters the mix as is very common, the whole picture becomes much more complex as can be seen in this photo.

A complex body shape has negative health consequences related to breathing, digestion, pain and overall function not to mention complexity of wheelchair seating.
The question is, can something be done beyond the wheelchair to address these problems?
References
Fulford, G.E., Brown, J.K. (1976). Position as a cause of deformity in cerebral palsy. Developmental Medicine and Child Neurology, 18, 305-14.
Gericke, T. (2006). Postural management for children with cerebral palsy: Consensus statement. Developmental Medicine & Child Neurology, 48(04), 244.
Hare Association for Physical Ability. Accessed June 2017.
Hill S., Goldsmith J. (2010) Biomechanics and Prevention of Body Shape Distortion. Tizard Learning Disability Review, 15 (2), 15-29.
Montana Postural Care Project. https://posture24-7.org/. Accessed June 2017.
Pope, P. (2007) Severe and Complex Neurological Disability: Management of the Physical Condition. Butterworth-Heinemann Publishers.
Tamara Kittelson-Aldred, MS, OTR/L, ATP/SMS
Project Director - Posture 24/7
Tamara Kittelson-Aldred is an occupational therapist, Assistive Technology Professional/Seating and Mobility Specialist. She earned certificates in advanced postural care through the Open College Network West Midlands in England. She directs the Montana Postural Care Project, promoting postural care and responsible wheelchair provision. Kittelson-Aldred has written and presented on these topics in the United States, Jordan, Peru, and Colombia and has served individuals with complex neurodisabilities in Montana since 1983. She credits her daughter Eleanore, born with cerebral palsy and profound deafness, as her best teacher.

