Prevention and Treatment at The Wheelchair Level
When we discuss Wound Care, it is natural for our minds to immediately jump to bedside prevention and treatment of a pressure injury. As health care providers–especially physicians, nurses, and specialized therapists in wound care–we understand bedside treatment well and find the appropriate support surface and techniques to promote healing and prevention of new pressure injuries. However, too often we forget a critical piece of the puzzle in the fight against pressure injuries: prevention and treatment at the wheelchair level!
This blog is meant to show how treatment techniques are just as critical from the seated posture as they are at bedside! The words you see above relate directly to wound care AS A WHOLE and make addressing the seated posture CRITICAL.
Our focus as a wound care team can no longer be to only treat bedside. Since our goal is to maximize our patient’s quality of life, we need to be able to safely position them out of the bed. We need to push to learn about, comprehend, and treat from wheelchair level as a complement to bedside treatment for optimal results. Understand that everything you have worked so hard to accomplish with cutting-edge bedside treatment can be undone in a matter of hours without the appropriate equipment choices at wheelchair level. We need to fully recognize the ramifications of general-use, entry-level products that are not designed to fight the extrinsic factors of wound development.
Did you know the common areas of skin breakdown are the same from both the bed and wheelchair? Compare the common areas of skin breakdown for yourself in the supine, semi-recumbent, and seated posture below.
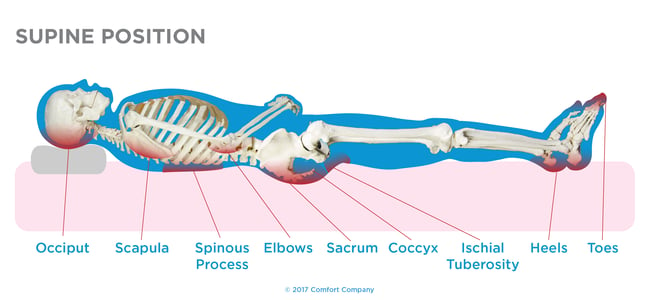
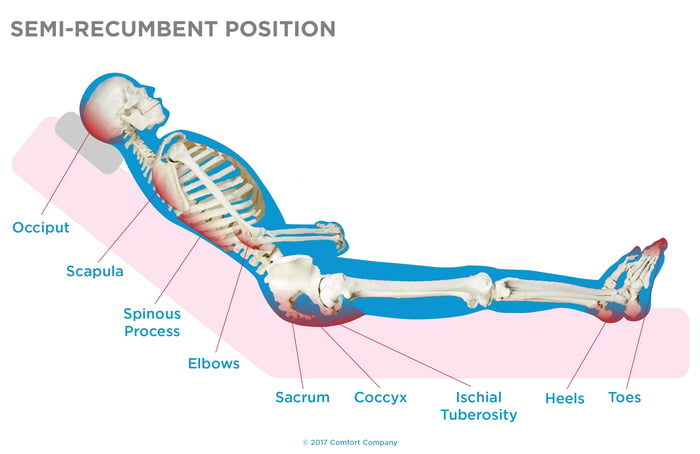
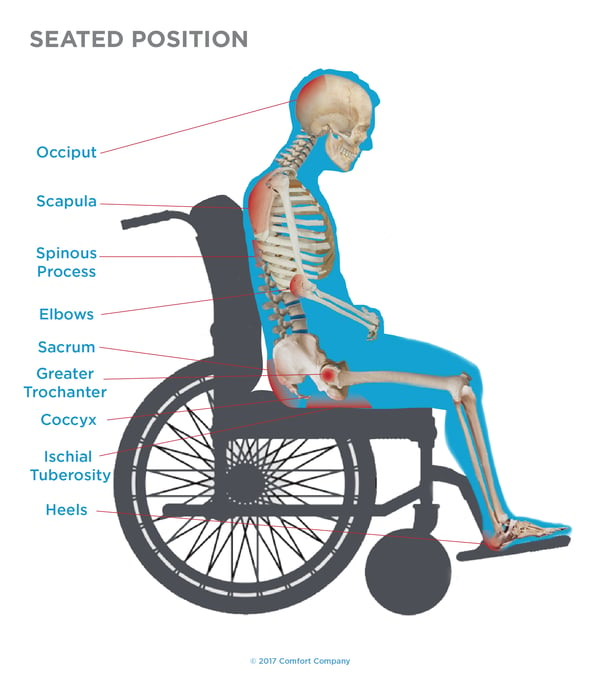
As you can clearly see, it only makes sense to give equal importance to providing the best equipment possible with all support surfaces.
In the wound care world we are trying to fight nasty extrinsic factors of pressure injury development,
- A pressure injury can develop in as little as an hour and four to six hours after sustained loading. (1)
- Our patients may be sitting all day on a low-quality cushion or back support, resulting in un-doing the healing progress made with bedside treatments.
Providers and facilities are just not as well versed when it comes to quality support surfaces for the wheelchair system and the role they play in treatment and prevention of a pressure injury. When we treat bedside and from the seated posture simultaneously, then and only then can we attack pressure, shear, and microclimate from every angle and minimize the risk of that dreaded pressure injury.
Are you ready to better protect and care for your patient with a pressure injury? Click here and use code comfort to take the webinar Wheelchair Seating and Positioning Misconceptions in Wound Care. Together we can increase our understanding of how the extrinsic factors relate to the seated posture. Let’s understand that by prescribing the appropriate skin protection cushions, back supports, and any needed accessories, we can minimize the risk of
1. Gefen, A. "How Much Time Does It Take to Get a Pressure Ulcer? Integrated Evidence from Human, Animal, and in Vitro Studies." Ostomy/wound Management.U.S. National Library of Medicine, Oct. 2008. Web. 20 July 2017.

Ana Endsjo, MOTR/L, CLT
Clinical Education Manager LTC Division
Ana Endsjo has worked as an occupational therapist since 2001 in a variety of treatment settings. She has mainly worked with the geriatric population, dedicated to the betterment of the treatment of the elderly in LTC centers. Her focus has been on seating and positioning and contracture management of the nursing home resident. With this experience, her hope is to guide other therapists, rehab directors, nurses, and administrators through educational guides, blogs, webinars, and live courses in her role as Clinical Education Manager for the long term care division.

