Part 5 in our series A to Z Considerations for Seating & Wheeled Mobility: A Quick Reference Clarifying Confusion Around CRT. See Part 1, Part 2, Part 3, Part 4, Part 5, Part 6, Part 7, Part 8, Part 9, Part 10, Part 11, Part 12, Part 13, Part 14, Part 15, Part 16, Part 17, Part 18, and Part 19.
Looking for more resources on seating and wheeled mobility? Check out our digital Wheelchair Seating and Positioning Guide.
Last week we talked all about the importance of the “interview” portion of the wheelchair evaluation, and this week we are going to look at the actual physical assessment and how it relates to seating and positioning and wheeled mobility. It is important to note that most of the information we need can be gathered from our “typical” PT/OT evaluation by looking at strength, balance, ROM, etc., and this is what we will be discussing in this week’s post. However, it is also critical that we complete a formal “mat assessment” where we also look at things like pelvic position, in seated and supine, and take measurements of hip width, upper leg length, etc. We need to discuss the client’s functional baseline and then, if possible, assess and trial the potential equipment. Your patient should demonstrate the ability to safely use the prescribed mobility equipment and show measurable functional increase compared to baseline. These are the items we will be discussing in the weeks to come!
Let’s dive in to our “typical” PT/OT assessment and look at how this information relates to wheeled mobility and potential seating and positioning needs. The following information will be synthesized to match the user to the appropriate mobility equipment:
- Muscle strength: Perform your typical manual muscle testing of ALL major muscle groups in both the upper and the lower extremities, being sure to include the hands/grip strength as this may impact the type of hand rim required to propel a manual wheelchair or possibly justify the need for a power wheelchair. Also, be sure to assess trunk and neck strength as this will be critical in the selection of the wheelchair and its components.
- Motor control: Assess the motor control/motor planning abilities of both the upper and lower extremities, including the hands, as well as of the trunk and neck. Does the client have the motor control to keep his/her hands on a hand rim to propel a manual wheelchair? Does he/she require a special type of hand rim or perhaps a power wheelchair to be safe and efficient? Can the client maintain his/her feet on the footplates, or do they have issues with lower extremity control? Can the client maintain the lower extremities in a neutral position, or do they lack motor control resulting in, perhaps, ABDuction and external rotation at the hips?
- Muscle tone: Is there increased or decreased muscle tone in the upper or lower extremities, trunk, or neck? If there is decreased tone, how does this effect posture and the ability to maintain a neutral sitting position? If there is increased tone, is it spasticity? Rigidity? Clonus? Identifying abnormalities in muscle tone and possible triggers of this tone is critical to provide equipment that will not only help to manage the tone but also to prevent the development or progression of postural abnormalities and contractures, if possible. It is also important to note that there are clients who use their increased tone for function; be sure to ask about this so we can take it into account in the device as our primary goal is increasing functional independence!
|
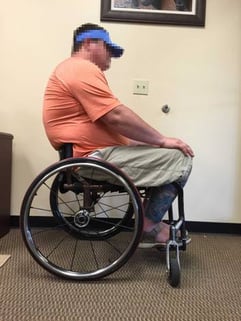
Decreased tone effecting the ability to maintain a neutral position |
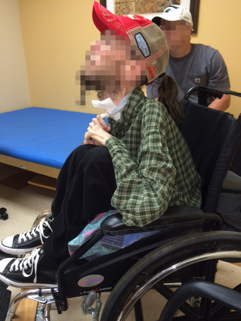
Increased tone effecting the ability to maintain a neutral position |
- Reflexes: Are there primitive reflexes that did not integrate due to a congenital condition or have re-surfaced due to a central nervous system injury? How do these reflexes impact movement and function?
- Skin integrity: Discuss any and all past and current pressure injuries, including stage 1 injuries and deep tissue injuries, and document the physical location as well as the stage of the injury. Remember that healed wounds are at an even higher risk for additional breakdown as the integrity of the skin is 80% what it was at baseline. Even a stage 1 (or a healed stage 1) pressure injury on the seated surfaces counts as qualifying an individual for a skin protection cushion! Be sure to also discuss any risk factors the client has for skin breakdown (i.e. lack of or impaired sensation on seated surfaces, incontinence issues, etc).
- Balance: Be sure to assess balance both in sitting and in standing, if possible. The client’s seated balance will help guide your cushion, back, and accessory choices depending on how much support he/she requires to maintain a neutral sitting posture (if able to achieve a neutral sitting posture based on ROM, pain, etc). For higher level patients who may need a wheeled mobility device due to multiple falls at home, consider performing an objective balance assessment such as the BERG or the Dynamic Gait Index (DGI) to assist you in the justification of the need.
- Range of Motion and Flexibility: Assess the range of motion in all joints in the upper and lower extremities, trunk, and neck. Be sure to assess these items in seated and in SUPINE. Supine is the only way we can eliminate the effects of gravity and get an accurate assessment of the flexibility of the pelvis, spine, and lower extremities.
In the next post, we will discuss the formal “mat assessment” and the “atypical” physical components of the wheelchair evaluation that you may not feel as comfortable or familiar with. Do NOT worry: while these items may feel a bit overwhelming at the surface, once we dig into them, you will find that you are fully capable of incorporating these items into your evaluation process! And, over time, you will become confident and efficient with that process.
Resources: Cole, Elizabeth, MSPT, ATP. “Steps in the Provision of Wheeled Mobility and Seating- Part 1.” U.S. Mobility; www.VGM.com.

Lindsey Sharpe, PT, DPT
Clinical Education Manager Rehab Division